Resources
New Study Examines the Relationship between Health Center Clinical, Financial, and Operational Excellence
Health centers are experiencing greater demands on their services as health reform implementation proceeds, often necessitating growth and operational transformation. As their role as key providers of primary care increases, health centers need to assess their current performance and develop strategies for improvement. Prior Capital Link studies have provided health centers, Primary Care Associations, and other stakeholders with insight into financial and operational trends. This analysis furthers our knowledge by examining the operating models, strategies, and practices of high-performing health centers to better understand the factors that work for and against the co-occurrence of strong clinical performance and financial sustainability.
This research sought to answer the following questions for the first time:
1. Do health centers that excel in providing high-quality patient care do better or worse than other health centers financially?
2. What are the characteristics of health centers that achieve both high-quality care and strong financial results?
3. What do high-performing health centers do differently or better than their peers?
The results of this analysis show that it is possible to reach quality targets while also performing well financially. Quality Awardee health centers achieve key quality targets and invest more in enabling staff and services, but are also able to produce strong financial results through revenue maximization, efficient medical care teams, and higher utilization through positive engagement with patients. The data further indicates that the highest performers have a greater ability to control costs—in particular, staffing costs—even though they are more heavily staffed with generally higher-cost physicians.
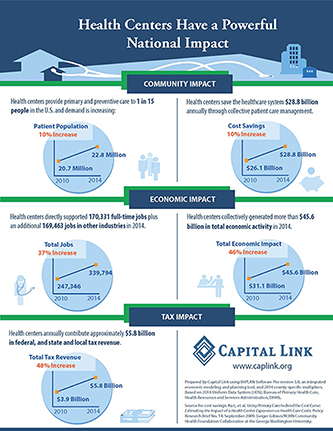
Key findings are illustrated in our infographic. Access a free download of the complete report at www.caplink.org/resources/publications.
New National Economic Impact Analysis and Special Pricing for State and Individual EIAs
Using economic modeling software, an Economic Impact Analysis (EIA) measures the effect a health center’s current operations has on the communities it serves, including job creation, tax impact, and cost savings. Health centers and PCAs have used this information in the past to educate policymakers, seek community support, and pursue funding opportunities.
In preparation for the upcoming NACHC Policy and Issues Forum, Capital Link updated the National Economic Impact Analysis with the latest data and is offering discounted pricing on our statewide and individual EIA reports. In order to receive your EIA before the P&I, you must submit all necessary information by February 28th. To find out more and order, please contact Steve Rubman, Director of Data and Information Systems, at This email address is being protected from spambots. You need JavaScript enabled to view it..
NACHC Payment Reform Readiness Assessment Tool
The NACHC Payment Reform Readiness Assessment Tool identifies key competency areas needed for successful health center engagement in the most prevalent and emerging payment reform models. It is designed to help health centers assess their current state of readiness, and to identify areas for improvement. The tool is not specific to one payer type or payment reform model. Rather, it is designed to capture core readiness areas that are needed for participation on in a variety of payment reform models in use by both public and private payers. The readiness assessment tool is designed to begin the conversation among health center leadership and staff about successful engagement in payment reform models. Access it here.
Brand new CHroniCles Website
CHroniCles, the dynamic, multi-media website dedicated to the living history of the community health center movement, is newly redesigned. The updated website improves overall user experience and allows visitors to better access the site on mobile and tablet devices. Check out the newly launched site here.
Coming Soon from Capital Link:
- Creating a Culture that Sustains a Patient-Centered Medical Home (Publication)
- Informing the Development of a Patient-Centered Medical Home Facility (Publication)
![]()